PrognoHealth – Corporate Health & Wellness Specialist
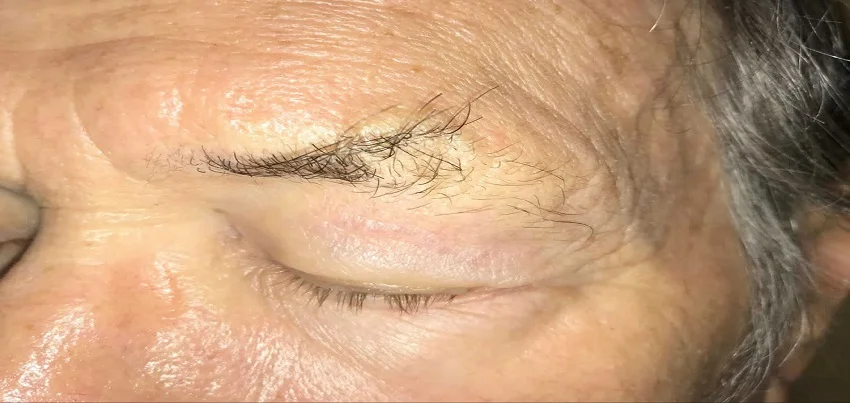
Madarosis Madarosis is a condition characterized by the loss of eyelashes or eyebrows. It can be caused by a variety of factors, including certain medical conditions, medications, and certain skin conditions. Symptoms of madarosis may include: Loss of eyelashes or eyebrows Thinning or patchy eyelashes or eyebrows Redness or itching of the eyelids Scaling or crusting of the eyelids Changes in the color or texture of the eyelashes or eyebrows To diagnose madarosis, a healthcare provider will typically perform a physical examination and ask about your symptoms. They may also order blood tests or a skin biopsy to confirm the diagnosis. The treatment for madarosis will depend on the underlying cause. In some cases, the condition may resolve on its own without treatment. However, if an underlying medical condition or medication is causing the madarosis, your healthcare provider will likely recommend treatment for that condition or a change in medication. If the madarosis is caused by a skin condition, such as eczema or psoriasis, your healthcare provider may recommend a topical cream or ointment to help with itching and inflammation. To prevent madarosis, it is important to take care of your eyelashes and eyebrows by: Avoiding harsh makeup or eyelash extensions Using a gentle, oil-free makeup remover Avoiding rubbing or pulling at your eyelashes or eyebrows Applying sunscreen to your eyelids to protect them from sun damage Annual health checkups are a great way to detect any potential health issues early, and corporate health and wellness programs can also play a key role in promoting preventative care and early detection of madarosis. A healthy diet and regular exercise can also help to boost your immune system and reduce your risk of developing madarosis. Eating a diet rich in fruits, vegetables, and whole grains can provide the nutrients your body needs to stay healthy. Exercise, such as walking, jogging, cycling, or swimming, can also help to keep your immune system strong. In conclusion, Madarosis is a condition characterized by the loss of eyelashes or eyebrows. It can be caused by a variety of factors, including certain medical conditions, medications, and certain skin conditions. The treatment for madarosis will depend on the underlying cause. To prevent madarosis, it is important to take care of your eyelashes and eyebrows, avoid harsh makeup or eyelash extensions, use a gentle, oil-free makeup remover, avoid rubbing or pulling at your eyelashes or eyebrows, apply sunscreen to your eyelids to protect them from sun damage. Annual health checkups and corporate health and wellness programs can play a key role in promoting preventative care and early detection of madarosis. A healthy diet and regular exercise can also help to boost your immune system and reduce the risk of developing madarosis. “Understanding Madarosis: Symptoms, Causes, Treatment, and Management Introduction: Madarosis refers to the loss or thinning of hair in the eyebrows or eyelashes, which can significantly impact an individual’s appearance and self-esteem. In this comprehensive guide, we will explore the symptoms, causes, treatment options, and management strategies for madarosis, providing insights into this distressing condition. Symptoms of Madarosis: Madarosis presents with the following symptoms: Loss or thinning of hair in the eyebrows or eyelashes Sparse or patchy areas where hair is absent Itching, irritation, or inflammation of the affected area Changes in the texture or color of the remaining hair Causes of Madarosis: Madarosis can be caused by various factors, including: Autoimmune diseases, such as alopecia areata or lupus Thyroid disorders, particularly hypothyroidism Dermatological conditions, including blepharitis or seborrheic dermatitis Medications, such as chemotherapy drugs or prostaglandin analogs Nutritional deficiencies, especially of vitamins or minerals essential for hair growth Allergic reactions to cosmetics or topical medications applied to the eyebrows or eyelashes Psychological stress or trauma, which can lead to hair-pulling behavior (trichotillomania) Treatment Options for Madarosis: Treatment for madarosis depends on the underlying cause and severity of the condition. Treatment options may include: Topical medications, such as corticosteroids or minoxidil, to stimulate hair growth Oral medications, such as immunosuppressants or thyroid hormones, to address underlying medical conditions Nutritional supplements, including biotin, vitamins, and minerals, to support hair health Lifestyle modifications, such as reducing stress or avoiding known allergens, to minimize exacerbating factors Surgical interventions, such as eyebrow transplants or eyelash extensions, for severe or cosmetically significant madarosis Management Strategies: In addition to treatment interventions, management of madarosis may involve: Regular follow-up appointments with a dermatologist or ophthalmologist to monitor progress and adjust treatment as needed Gentle cleansing and care of the affected area to prevent further irritation or damage to the hair follicles Psychological support and counseling for individuals experiencing emotional distress or self-esteem issues related to madarosis Education and awareness initiatives to promote understanding of madarosis and reduce stigma associated with hair loss conditions Madarosis Madarosis refers to the loss or absence of eyelashes and/or eyebrows. This condition can occur due to various underlying causes and can affect one or both sides of the face. It’s important to diagnose the underlying cause accurately to manage the condition effectively. Types of Madarosis Madarosis can be categorized based on the location and pattern of hair loss:1. Ciliary Madarosis: Loss of eyelashes.2. Superciliary Madarosis: Loss of eyebrows.3. Unilateral Madarosis: Hair loss on one side.4. Bilateral Madarosis: Hair loss on both sides. Causes of Madarosis Madarosis can result from a wide range of factors, including dermatological, systemic, infectious, and traumatic causes. Here’s a detailed look at the possible causes: 1. Dermatological Conditions:o Alopecia Areata: An autoimmune disorder causing patchy hair loss on the scalp, eyebrows, and eyelashes.o Seborrheic Dermatitis: An inflammatory condition that can cause scaling and loss of hair.o Psoriasis: Can lead to scaling and hair loss in the affected areas.o Atopic Dermatitis: Chronic skin inflammation that may affect hair-bearing areas.o Lichen Planus: An inflammatory condition affecting skin, hair, and mucous membranes.2. Systemic Conditions:o Thyroid Disorders: Both hyperthyroidism and hypothyroidism can lead to hair loss, including eyelashes and eyebrows.o Nutritional Deficiencies: Deficiencies in vitamins (like Vitamin B7 or Biotin, Vitamin D), minerals (such as zinc, iron), or protein can
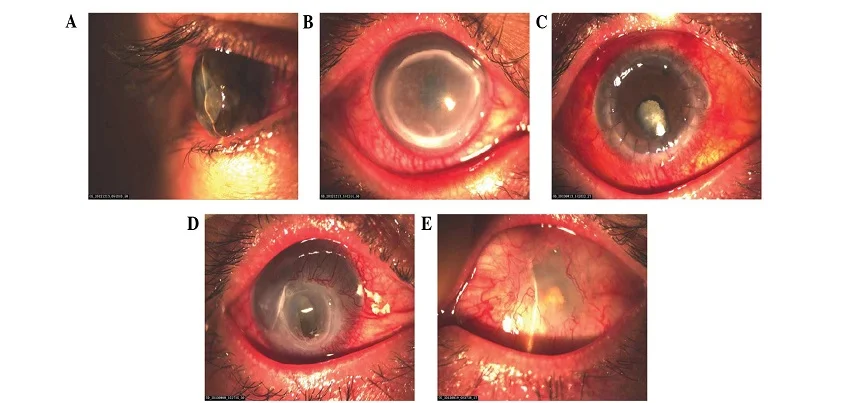
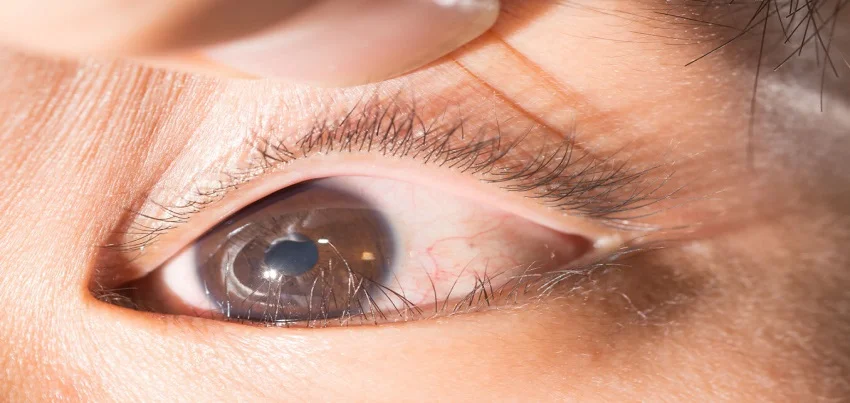
Read MoreMooren’s Ulcer Mooren’s ulcer is a rare, chronic, progressive and recurrent condition characterized by the formation of an ulcer on the cornea of the eye. The exact cause of Mooren’s ulcer is unknown, however, it is believed to be an autoimmune disorder that causes inflammation and destruction of the cornea. Symptoms of Mooren’s ulcer include pain, redness, tearing, and blurred vision. In some cases, the ulcer can lead to vision loss or even blindness if left untreated. The ulcer usually starts as a small, circular, grayish white lesion on the cornea, which then enlarges and becomes more irregular in shape. Diagnosis of Mooren’s ulcer typically involves a thorough eye examination, including a slit-lamp examination and a corneal scraping to obtain a sample of the ulcer for analysis. Imaging tests such as ultrasound, or in some cases, a biopsy may also be used to confirm the diagnosis. Treatment for Mooren’s ulcer typically involves a combination of therapies, including topical and oral corticosteroids, immunosuppressive agents, and antibiotics to prevent secondary infection. In some cases, surgical intervention such as corneal transplantation may be required to restore vision. Preventing Mooren’s ulcer is key to maintaining good eye health. Annual health check-ups can help identify potential risk factors for Mooren’s ulcer, such as autoimmune disorders, and provide an opportunity to discuss prevention strategies with a healthcare provider. Corporate health and wellness programs can also help to promote healthy habits among employees, such as regular exercise, healthy eating, and stress management, which can have a positive impact on eye health. Diet and exercise are key components of preventing Mooren’s ulcer. Eating a diet rich in fruits, vegetables, whole grains, and lean proteins can help to lower the risk of eye damage. Regular exercise, such as brisk walking or cycling, can also help to improve eye function. It is important to keep your weight in check, as obesity is a major risk factor for eye disease. In addition to regular check-ups, corporate health and wellness programs can also help to promote healthy habits among employees, such as regular exercise, healthy eating, and stress management. These programs can include things like on-site fitness classes, healthy food options in the workplace, and stress management resources. In conclusion, Mooren’s ulcer is a rare, chronic, progressive and recurrent condition characterized by the formation of an ulcer on the cornea of the eye, which can lead to vision loss or even blindness if left untreated. The cause of Mooren’s ulcer is unknown, however, it is believed to be an autoimmune disorder. Treatment for Mooren’s ulcer typically involves a combination of therapies, including topical and oral corticosteroids, immunosuppressive agents, and antibiotics. Preventing Mooren’s ulcer is key to maintaining good eye health. Annual health check-ups, corporate health and wellness programs, diet, and exercise can all play a role in preventing Mooren’s ulcer. It is important to be aware of the risk factors and take steps to lower your risk. With appropriate care and management, Mooren’s ulcer can be prevented, and the risk of complications can be reduced.
Read MoreLagophthalmos Lagophthalmos is a condition in which the eyelids are unable to close completely, leaving the eye exposed and unprotected. This can lead to a variety of symptoms, including dry eyes, irritation, and even vision loss. Symptoms of Lagophthalmos can vary depending on the severity of the condition. They can include dry eyes, itching, redness, blurred vision, and even double vision. In severe cases, the eye may be exposed to air and light during sleep, leading to corneal damage and inflammation. Diagnosis of Lagophthalmos is typically made through a physical examination, during which the physician will look for signs of eyelid malposition and assess the affected area for any changes in skin texture or color. They may also use a special instrument called a caliper to measure the distance between the cornea and the eyelid. Other diagnostic tests that may be used include eyelid photography, which uses a special camera to capture images of the eyelids, and corneal topography, which uses a special device to map the shape of the cornea. Treatment for Lagophthalmos can vary depending on the underlying cause of the condition, but common treatment methods include eyelid surgery, also known as blepharoplasty. This procedure involves repositioning the eyelids to their proper position. In some cases, additional procedures, such as Botox injections, or temporary eyelid taping, may be used to help the eyelids heal. In some cases, the use of punctal plugs, which are small devices inserted into the tear ducts to reduce tear drainage and prevent dry eyes, can also be useful. Prevention of Lagophthalmos is the key to avoid the condition and its symptoms. This is where annual health check-ups and corporate health & wellness programs come in. These programs can help you identify any potential risks for Lagophthalmos, such as a family history of the condition, and take steps to prevent it from occurring. For example, if you are at risk for Lagophthalmos, your doctor may recommend that you avoid certain activities that could put extra pressure on your eyelids, such as heavy lifting or carrying heavy bags. In addition to taking care of your health, there are also a few lifestyle changes that can help to prevent Lagophthalmos. One of the most important things you can do is to maintain a healthy diet and exercise regularly. Eating a diet that is low in fat and high in fiber can help to reduce your risk of Lagophthalmos, as can regular exercise, which can help to improve the function of your eyelids. In conclusion, Lagophthalmos is a condition in which the eyelids are unable to close completely, leaving the eye exposed and unprotected. It can cause a variety of symptoms, including dry eyes, irritation, and even vision loss. It can be diagnosed through physical examination and other diagnostic tests. Treatment options include eyelid surgery, Botox injections, or temporary eyelid taping and punctal plugs. To prevent Lagophthalmos, it is essential to take care of your health through annual health check-ups and corporate health & wellness programs, maintain a healthy diet and exercise regularly.
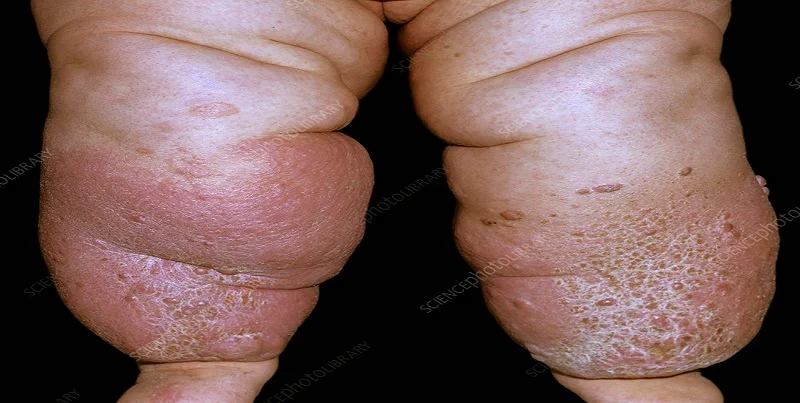
Read MoreLymphoedema Lymphoedema is a chronic condition that occurs when the lymphatic system, which is responsible for draining excess fluid from the body’s tissues, is not functioning properly. This can lead to swelling and discomfort in the affected area. Symptoms of lymphoedema include swelling, pain, tightness of the skin, and a feeling of heaviness. Diagnosis of lymphoedema is typically made through a physical examination, during which the physician will look for signs of swelling and assess the affected area for any changes in skin texture or color. They may also use a tape measure to measure the circumference of the affected limb or area. Other tests that may be used to diagnose lymphoedema include lymphoscintigraphy, which uses a special dye to visualize the lymphatic vessels, and bioimpedance spectroscopy, which measures the amount of fluid in the affected area. There are several treatment options available for lymphoedema, and the best course of treatment will depend on the individual case. The most common treatment methods include compression therapy, which uses compression garments to reduce swelling and promote lymphatic flow, and manual lymphatic drainage, which uses massage to help move lymphatic fluid out of the affected area. Other treatments that may be used include skin care, exercise, and elevation of the affected limb. One of the best ways to prevent lymphoedema is to take care of your health, and this is where annual health check-ups and corporate health & wellness programs come in. These programs can help you identify any potential risks for lymphoedema, such as a family history of the condition, and take steps to prevent it from occurring. For example, if you are at risk for lymphoedema, your doctor may recommend that you avoid certain activities that could put extra pressure on your lymphatic system, such as heavy lifting or carrying heavy bags. In addition to taking care of your health, there are also a few lifestyle changes that can help to prevent lymphoedema. One of the most important things you can do is to maintain a healthy diet and exercise regularly. Eating a diet that is low in fat and high in fiber can help to reduce your risk of lymphoedema, as can regular exercise, which can help to improve the function of your lymphatic system. In conclusion, lymphoedema is a chronic condition that can cause swelling and discomfort in the affected area. It can be diagnosed through physical examination and other tests, and treated with compression therapy, manual lymphatic drainage, skin care, exercise, and elevation of the affected limb. To prevent lymphoedema, it is essential to take care of your health through annual health check-ups and corporate health & wellness programs, maintain a healthy diet and exercise regularly.
Read MoreHorner Syndrome Horner Syndrome is a disorder of the sympathetic nervous system that affects the eye, face and neck. It is characterized by a combination of symptoms that include a drooping eyelid, a small pupil, and a lack of sweating on one side of the face. It can be caused by a variety of underlying conditions such as a tumor, injury, or disease. Symptoms of Horner Syndrome include a drooping eyelid, a small pupil, and a lack of sweating on one side of the face, along with the absence of wrinkles on the forehead. Other symptoms can include redness of the eye, dryness of the eye, and sensitivity to light. Diagnosis of Horner Syndrome typically begins with a physical examination and a neurological examination to evaluate the pupil, eyelid, and sweating. Additional tests such as a CT scan or MRI may be performed to identify the underlying cause of the condition. Treatment of Horner Syndrome depends on the underlying cause of the condition. In some cases, no treatment may be necessary, while in others, treatment may include medications, such as epinephrine, to dilate the pupil, or surgery to remove a tumor or repair an injury. Preventing Horner Syndrome is not possible as it is a disorder caused by various underlying conditions. However, early diagnosis and appropriate treatment can help to prevent serious complications and improve quality of life. During an annual health check-up, it is important to have a thorough physical examination and neurological examination to detect any signs of Horner Syndrome and take steps to prevent it from occurring. Corporate health and wellness programs can also play a role in supporting employees who have Horner Syndrome by providing access to appropriate care and resources. Diet and exercise do not prevent Horner Syndrome, but maintaining a healthy diet and regular physical activity can help to maintain overall health and well-being. Eating a balanced diet that is rich in fruits, vegetables, and lean proteins can help to support the body and improve overall health. Exercise can also help to improve cardiovascular health, boost the immune system, and reduce stress. In conclusion, Horner Syndrome is a disorder of the sympathetic nervous system that affects the eye, face and neck. By understanding the symptoms, getting regular check-ups and appropriate treatment, it is possible to prevent serious complications and improve quality of life. Corporate health and wellness programs can also play a key role in supporting employees who have Horner Syndrome by providing access to appropriate care and resources.
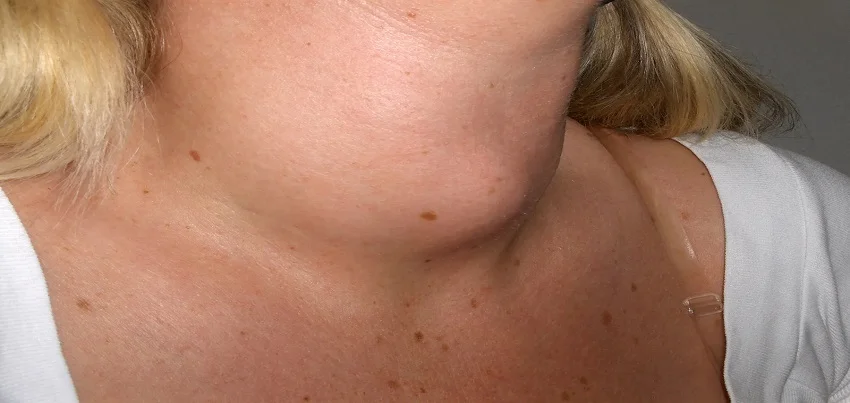
Read MoreGoitre Goitre is a condition characterized by the enlargement of the thyroid gland, which is located in the front of the neck. The thyroid gland produces hormones that regulate the body’s metabolism, so an enlarged thyroid gland can lead to a variety of symptoms, including difficulty swallowing, hoarseness, and difficulty breathing. In some cases, the goitre may be visible as a lump in the neck. Symptoms of goitre can vary depending on the underlying cause of the condition. Common symptoms include an enlarged thyroid gland, which may be visible as a lump in the neck, difficulty swallowing, hoarseness, and difficulty breathing. Goitre can also cause fatigue, weight gain or loss, and changes in the menstrual cycle for women. A physical examination, blood tests, and imaging tests are commonly used to diagnose goitre. A physical examination involves a doctor or healthcare professional looking at the neck and feeling for an enlarged thyroid gland. Blood tests such as TSH (thyroid-stimulating hormone) and T4 (thyroxine) are used to check the levels of hormones produced by the thyroid gland. If a lump is felt during examination, an ultrasound, CT scan or MRI may be ordered to get a clear view of the thyroid gland and to confirm the diagnosis. The treatment of goitre depends on the underlying cause of the condition. If the goitre is caused by an iodine deficiency, then supplementing the diet with iodine may help to reduce the size of the thyroid gland. If the goitre is caused by an overactive thyroid, then medications such as antithyroid drugs or radioactive iodine may be used to slow down the thyroid’s hormone production. In some cases, surgery may be necessary to remove all or part of the thyroid gland. Preventing goitre from occurring is challenging as the underlying causes of goitre can vary. However, certain risk factors have been identified, including a family history of goitre, radiation exposure, and certain autoimmune disorders. People with these risk factors should be especially vigilant about getting regular check-ups and annual health check-ups to detect any abnormalities in the thyroid gland. In addition to regular check-ups, a healthy diet and regular exercise can also help to reduce the risk of developing goitre. Eating a diet that is rich in fruits, vegetables, and whole grains can help to lower the risk of developing the disease. Regular physical activity, such as walking or cycling, can also help to improve overall health and reduce the risk of developing goitre. Corporate health and wellness programs can play a key role in preventing goitre by encouraging regular check-ups and annual health check-ups. These programs can also promote healthy lifestyle behaviors, such as regular exercise and a healthy diet, which can help to reduce the risk of developing the disease. In summary, Goitre is a condition characterized by the enlargement of the thyroid gland, which can lead to a variety of symptoms. The diagnosis of goitre can be done through physical examination, blood tests, and imaging tests. The treatment of goitre depends on the underlying cause of the condition which can range from medication, radioactive iodine or surgery. Prevention of goitre is challenging, but regular check-ups, healthy diet, and regular exercise can help reduce the risk of developing the disease. Corporate health and wellness programs can also play a key role in preventing goitre by encouraging regular check-ups and healthy lifestyle behaviors.
Read MoreGastro-Esophageal Reflux Disease (GERD) Gastro-Esophageal Reflux Disease (GERD) is a common condition that affects millions of people worldwide. It is characterized by a burning sensation in the chest, known as heartburn, and can also lead to other symptoms such as acid reflux, coughing, and difficulty swallowing. Symptoms of GERD can vary from person to person, but common signs include heartburn, acid reflux, and chest pain. Other symptoms may include coughing, difficulty swallowing, and a sour taste in the mouth. These symptoms can be caused by a variety of factors, including a malfunctioning lower esophageal sphincter, which is the muscle that helps to keep stomach acid from flowing back into the esophagus. To diagnose GERD, a physician may perform a number of tests, including an endoscopy, which is a procedure that allows the doctor to examine the inside of the esophagus and stomach using a small camera. Other tests that may be used to diagnose GERD include a barium swallow or a pH monitoring test, which measures the acidity of the stomach. Treatment for GERD typically involves a combination of lifestyle changes and medication. Common medications used to treat GERD include proton pump inhibitors (PPIs), which reduce the amount of acid produced by the stomach, and H2 receptor blockers, which block the action of histamine, a chemical that stimulates the production of stomach acid. To prevent GERD from occurring, there are a number of lifestyle changes that can be made. These include avoiding foods and drinks that may trigger symptoms, such as coffee, chocolate, and spicy foods, as well as maintaining a healthy diet and exercise routine. Additionally, smoking and drinking alcohol should be avoided, as they can aggravate GERD symptoms. Annual health check-ups and corporate health & wellness programs can also play an important role in preventing GERD. These programs can help to identify individuals at risk for GERD and provide them with the necessary resources and support to make lifestyle changes that can help to reduce their risk. In addition to the above, making dietary changes can also help to prevent GERD from occurring. Eating smaller, more frequent meals, rather than large meals, can help to reduce the amount of acid produced by the stomach. Additionally, avoiding foods and drinks that may trigger symptoms, such as coffee, chocolate, and spicy foods, can also be helpful. Exercise is also a key component in preventing GERD. Regular physical activity can help to improve the functioning of the lower esophageal sphincter, which can help to reduce the risk of acid reflux. Additionally, maintaining a healthy weight can also help to reduce the risk of GERD, as obesity is a known risk factor for the condition. In conclusion, Gastro-Esophageal Reflux Disease (GERD) is a common condition that affects millions of people worldwide. It is characterized by symptoms such as heartburn, acid reflux, and chest pain. To diagnose GERD, a physician may perform a number of tests, including an endoscopy. Treatment for GERD typically involves a combination of lifestyle changes and medication. To prevent GERD from occurring, there are a number of lifestyle changes that can be made, such as avoiding foods and drinks that may trigger symptoms, and maintaining a healthy diet and exercise routine. Annual health check-ups and corporate health & wellness programs can also play an important role in preventing GERD. Additionally, making dietary changes, such as eating smaller, more frequent meals and avoiding foods that may trigger symptoms and regular physical activity can also help to prevent GERD
Read MoreEpicanthus Epicanthus is a congenital condition characterized by a fold of skin that covers the inner corner of the eye. This fold of skin can cause the eyelashes to rub against the cornea, leading to a variety of symptoms including redness, itching, and discomfort in the affected eye. In some cases, epicanthus can also lead to vision problems or even permanent damage to the cornea. The symptoms of epicanthus are relatively easy to identify. The most common symptoms include redness and itching in the affected eye, as well as discomfort and a sensation of something being in the eye. In some cases, people with epicanthus may also experience vision problems, such as blurriness or double vision. The fold of skin on the inner corner of the eye is also visible. If you suspect that you may have epicanthus, it is important to visit an eye doctor for a proper diagnosis. The most common tests used to diagnose epicanthus include a thorough examination of the eye and eyelid, as well as tests to measure the curvature of the cornea. The doctor may also take a family history and examine the child’s other facial features as it can be related to other conditions like Down syndrome. Treatment for epicanthus typically depends on the severity of the case and can include a combination of methods, including the use of eye drops or ointments to reduce redness and itching, as well as the use of special eye patches or other devices to keep the eyelashes from rubbing against the cornea. In severe cases, surgery may be necessary to correct the underlying problem and prevent further damage to the eye. The surgery is called epicanthoplasty, which involves the removal of the skin fold and repositioning of the eyelid. Preventing epicanthus from occurring in the first place is not possible as it is a congenital condition. However, practicing good eye hygiene, including regular cleaning of the eyelashes and eyelids, as well as avoiding anything that might irritate the eyes, such as smoke or dust can help to reduce the symptoms. Diet and exercise do not play a direct role in preventing epicanthus as it is a congenital condition. However, a healthy diet and regular exercise can help to improve overall health, which can in turn help to reduce the risk of other eye problems. Annual health check-ups and corporate health & wellness programs are a great way to stay on top of your eye health and catch any potential problems early on. During an annual health check-up, your eye doctor will perform a thorough examination of your eyes and eyelids, looking for any signs of epicanthus or other eye problems. Corporate health & wellness programs can also provide employees with regular eye exams, as well as education on eye health and the importance of regular check-ups. In conclusion, Epicanthus is a congenital condition characterized by a fold of skin that covers the inner corner of the eye. The fold of skin can cause the eyelashes to rub against the cornea, leading to a variety of symptoms including redness, itching, and discomfort in the affected eye. Preventing epicanthus from occurring is not possible as it is a congenital condition. However, good eye hygiene can help to reduce the symptoms. Annual health check-ups and corporate health & wellness programs are a great way to stay on top of your eye health and catch any potential problems early on. If you suspect that you may have epicanthus, it is important to visit an eye doctor for a proper diagnosis and treatment.
Read MoreEpiblepharon Epiblepharon is a condition in which the eyelid skin and muscle tissue fold over the eyelashes, causing them to rub against the cornea. This can lead to a variety of symptoms, including redness, itching, and discomfort in the affected eye. In some cases, epiblepharon can also lead to vision problems or even permanent damage to the cornea. The symptoms of epiblepharon are relatively easy to identify. The most common symptoms include redness and itching in the affected eye, as well as discomfort and a sensation of something being in the eye. In some cases, people with epiblepharon may also experience vision problems, such as blurriness or double vision. If you suspect that you may have epiblepharon, it is important to visit an eye doctor for a proper diagnosis. The most common tests used to diagnose epiblepharon include a thorough examination of the eye and eyelid, as well as tests to measure the curvature of the cornea. Treatment for epiblepharon typically involves a combination of methods, including the use of eye drops or ointments to reduce redness and itching, as well as the use of special eye patches or other devices to keep the eyelashes from rubbing against the cornea. In some cases, surgery may be necessary to correct the underlying problem and prevent further damage to the eye. Preventing epiblepharon from occurring in the first place is the best way to protect your eyes and vision. One of the most effective ways to do this is to practice good eye hygiene, including regular cleaning of the eyelashes and eyelids, as well as avoiding anything that might irritate the eyes, such as smoke or dust. Diet and exercise can also play a role in preventing epiblepharon. Eating a healthy diet that is rich in vitamins and minerals, particularly those that are good for the eyes, such as vitamin A and omega-3 fatty acids, can help to strengthen the eye and reduce the risk of epiblepharon. Additionally, regular exercise can help to improve overall health, which can in turn help to reduce the risk of eye problems. Annual health check-ups and corporate health & wellness programs are a great way to stay on top of your eye health and catch any potential problems early on. During an annual health check-up, your eye doctor will perform a thorough examination of your eyes and eyelids, looking for any signs of epiblepharon or other eye problems. Corporate health & wellness programs can also provide employees with regular eye exams, as well as education on eye health and the importance of regular check-ups. In conclusion, Epiblepharon is a condition in which the eyelid skin and muscle tissue fold over the eyelashes, causing them to rub against the cornea. Preventing epiblepharon from occurring in the first place is the best way to protect your eyes and vision. Good eye hygiene, healthy diet, regular exercise, annual health check-ups and corporate health & wellness programs can help to reduce the risk of epiblepharon and other eye problems. If you suspect that you may have epiblepharon, it is important to visit an eye doctor for a proper diagnosis and treatment.
Read MoreEpidemic Dropsy Epidemic dropsy, also known as beriberi, is a disease caused by a deficiency of vitamin B1, also known as thiamine. The disease is characterized by symptoms such as weakness, fatigue, and numbness in the limbs, as well as heart and nerve damage. The symptoms of epidemic dropsy can vary depending on the severity of the deficiency. Early symptoms may include fatigue, weakness, and numbness or tingling in the limbs. As the deficiency progresses, symptoms may include difficulty walking, loss of muscle function, and heart and nerve damage. In severe cases, the disease can lead to paralysis, coma, and death. Diagnosis of epidemic dropsy typically involves a physical examination and a series of tests, including blood tests to measure thiamine levels and imaging tests to check for heart and nerve damage. Treatment for epidemic dropsy typically involves administering thiamine supplements to correct the deficiency. In cases of severe deficiency, thiamine may be given by injection. In addition, treatment may also include physical therapy to help improve muscle function and prevent complications. Prevention of epidemic dropsy is key, and can be achieved through a diet that is rich in thiamine. Foods such as whole grains, nuts, and seeds are good sources of thiamine. In addition, regular exercise and annual health check-ups are important in preventing the disease. Corporate health and wellness programs can also play a role in preventing epidemic dropsy by promoting healthy eating and exercise habits among employees. In terms of diet and exercise to prevent epidemic dropsy, incorporating foods high in thiamine such as whole grains, nuts, and seeds into your diet is important. It is also important to maintain a healthy weight through regular exercise. Corporate health and wellness programs can also help in preventing the disease by promoting healthy eating and exercise habits among employees. Annual health check-ups are also an important tool in preventing epidemic dropsy. These check-ups can identify any potential deficiencies early on and allow for prompt treatment to prevent the disease from progressing. Corporate health and wellness programs can also play a role by promoting regular check-ups among employees. In conclusion, epidemic dropsy is a serious disease caused by a deficiency of vitamin B1. It is characterized by symptoms such as weakness, fatigue, and numbness in the limbs. Diagnosis typically involves a physical examination and a series of tests, including blood tests to measure thiamine levels and imaging tests to check for heart and nerve damage. Treatment typically involves administering thiamine supplements to correct the deficiency. Prevention can be achieved through a diet that is rich in thiamine, regular exercise, annual health check-ups and Corporate health & wellness programs. It is important to take preventive measures to avoid this serious disease.
Read More